Any interruption to the correct/normal storage of frozen exhibits needs to be recorded in as much detail as possible (see below).
The items would still be assessed by the forensic scientist, almost regardless of the interruption. A decision would then be made about testing. In most cases the testing would go ahead, but the information about the interruption, and the visible state of the items/swabs would inform the evaluation of the findings.
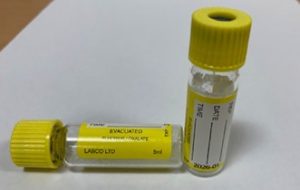
Toxicology samples
In relation to toxicology samples. Some drugs are still stable at room temperature but alcohol and some drugs do degrade over time and this degradation will be quicker at room temperature. Alcohol can also be produced in samples – if certain micro-organisms are present.
There are many variables such as whether the degradation is from microbial action or simply heat, how warm the samples get, the length of time that the samples are above recommended freezer (or refrigerated) temperature, the concentration of alcohol and drugs in the sample and whether or not the degradation products would also be detected by the analysis. For most drugs, it is unlikely that a high concentration would decrease to undetectable levels but, in a case with long time intervals where there may be drugs around the detection limit, some drugs could degrade to undetectable levels.
The toxicologist would generally continue with the analysis but add caveats to the results depending on the drug suspected and the circumstances of the case. Ideally, information regarding how warm the freezer (or fridge) got and for how long would be required. Fridge/freezer monitoring should be in place and regularly checked.
Samples that are to be submitted for toxicology analysis within a few weeks can generally be stored refrigerated or frozen so, if a freezer breaks down and the temperature does not exceed refrigerated temperatures before it is noticed, then this should not be an issue.
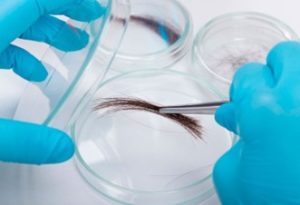
Biological samples for DNA
The time taken from ambient storage to freezing of swabs is possibly less critical than the amount of time a sample is frozen or thawed but either way minimising extremes of temperature change is good practice.
Guidance on fridge/freezer monitoring
Monitoring the temperature of the fridge and/or freezer with a daily check recorded is essential for a complete record of temperature at which the sample has been stored including any temperature deviations. The actual acceptable temperature range appears to be governed by what is specified by the equipment manufacturer e.g. fridges operate at 2° to 8° C and freezers operate at approximately -20 °C (must be below -10 °C to maintain freezing).
Best practice is to check the freezer temperatures daily and record the reading. Action is required if the temperature deviates up or down by 5 °C. Freezers should be alarmed and there should be a backup generator. It is good practice for the equipment used for the temperature monitoring to be calibrated and its accuracy known.
It is possible where freezers have broken down or have been accidentally switched off for up to 48 hours that there may still be positive body fluid findings and DNA results.
The storage of toxicology samples is non critical i.e. it just needs to be at ‘refrigerated’ or ‘frozen’ temperatures but does not need to be at a specific temperature (as it may need to be for certain diagnostic reagents, some medications, certain foods etc).